Why full-body MRI screening is surging online, and what Houston doctors say it can’t promise
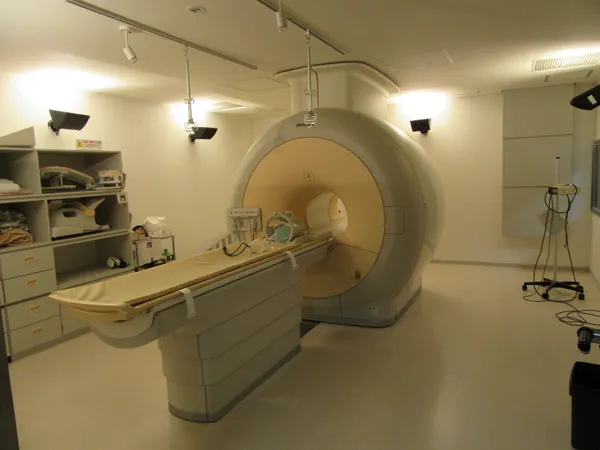
A rapidly expanding, self-pay scan enters the mainstream health conversation
Full-body MRI screening—marketed as a one-visit scan of major organs to identify hidden disease—has become a fast-growing wellness purchase promoted widely on social media. The trend has accelerated alongside direct-to-consumer imaging companies offering elective scans outside traditional medical pathways, often paid out of pocket.
In Houston, the conversation is increasingly driven by stories of individuals who pursued a scan after persistent symptoms or as a precaution. In one recent account, a Houston father said a full-body MRI led to the discovery of an underlying condition after months of unexplained exhaustion, changing the direction of his care and day-to-day life.
What a “full-body MRI” typically covers—and what it can miss
Whole-body MRI protocols generally image multiple regions such as the head/neck, chest, abdomen and pelvis in a single session. While MRI avoids ionizing radiation, it is not a universal “all cancers, all diseases” detector. Detection depends on scan protocol, image resolution, and whether a condition produces changes visible on MRI at the time of scanning.
Clinical specialists note that some diseases may be difficult to evaluate with broad screening protocols, and certain organs or conditions may require dedicated, targeted imaging or other screening tests to be assessed reliably. A normal scan also does not guarantee that significant disease will not develop or be discovered later.
Medical consensus: limited evidence for routine screening in low-risk, symptom-free people
Major radiology organizations have publicly stated that evidence is currently insufficient to recommend total-body MRI screening for people without symptoms or specific risk factors. These statements emphasize the lack of proof that such screening is cost-effective or improves longevity in average-risk populations, and they warn about downstream consequences from non-specific findings.
By contrast, whole-body MRI can have an established role in selected high-risk situations, including some inherited cancer predisposition syndromes and certain oncology applications where broad staging or surveillance is clinically indicated.
The central tradeoff: early detection versus incidental findings and follow-up cascades
A recurring challenge in broad imaging is the frequency of incidental findings—unexpected abnormalities that may be benign or of uncertain significance. Population studies and systematic reviews have documented that incidental findings are common in whole-body MRI screening, and that a subset can trigger additional imaging, specialist consultations, and, in some cases, biopsies. Research has also linked disclosure of incidental findings to increased subsequent health-service use and costs in general-population cohorts.
For patients, the practical implication is that a screening scan can shift uncertainty rather than eliminate it: some findings lead to clear next steps, while others require weeks or months of surveillance or further testing to rule out serious disease.
What patients should clarify before booking
- Whether symptoms or personal/family history suggest targeted testing is more appropriate than broad screening.
- Exactly which body regions are imaged, what is excluded, and whether contrast is used.
- Who reads the scan (board-certified radiologist), how findings are categorized, and how follow-up is coordinated.
- Expected rates of incidental findings and the likely downstream steps if something indeterminate appears.
- Total costs beyond the scan itself, including potential additional imaging, appointments, or procedures.
As full-body MRI screening spreads online, clinicians and patients are confronting the same question: when does more information improve health outcomes, and when does it primarily generate additional testing?
For Houston-area families weighing an elective scan, the most consequential details often emerge after the appointment is made: what the test can realistically detect, how often it uncovers ambiguous findings, and whether the result will change medical management.
Harris County investigators respond after reported tank fire at Sheldon Road refinery in East Houston area

Planned Ritz-Carlton tower in Uptown Houston targets $30 million-plus condos, testing local price records
Houston-area family seeks US assistance as Qatar airspace closures strand Americans amid Iran conflict escalation
